Forty years ago, researchers described the mysterious cases of five gay men who had fallen ill with a pneumonia caused by the fungus Pneumocystis carinii. Two of the five men had already died.
That type of pneumonia usually affects only individuals who are severely immunocompromised, researchers wrote in the June 5, 1981 Morbidity and Mortality Weekly Report. Scientists would soon discover that a disease that would come to be known as AIDS was devastating the men’s immune systems.
Three years later, scientists pinned the blame for AIDS on a virus dubbed HIV, or human immunodeficiency virus. Margaret Heckler, the then-U.S. Secretary of Health and Human Services, said in an April 1984 news conference that a vaccine to build protection against the virus would be ready to test within two years, holding out promise that protection was on its way.
We’re still waiting.
Meanwhile, the HIV pandemic, which probably got its start in Congo in the 1920s, has led to devastating loss. More than 75 million people have been infected around the world as of the end of 2019. Approximately 32.7 million people have died.
That toll would undoubtedly be much higher if it weren’t for advances in antiviral treatments that can prevent infected people from dying from HIV and from transmitting the virus to others (SN: 3/4/20; SN: 11/15/19). To date, only three people have beaten an HIV infection (SN: 8/26/20). For most, it lasts a lifetime.
That long-lasting infection is just one reason why no vaccine against HIV exists yet. It’s also a tricky virus to pin down, with many variants and an uncanny ability to evade the immune system.
And money is an issue too. The lack of an effective HIV vaccine stands in stark contrast to COVID-19 vaccines that took less than a year to develop (SN: 11/9/20). For COVID-19 vaccine development, “the money poured in, which was the right thing to do,” says Susan Zolla-Pazner, an immunologist at the Icahn School of Medicine at Mount Sinai in New York City. Funding for HIV vaccine research comes in five-year installments, making it difficult to allocate the money in an efficient way to get a vaccine off the ground. Still, that funding stream has allowed for advances in HIV research, which partly enabled the rapid success of multiple COVID-19 vaccines.
The technology behind Johnson & Johnson’s COVID-19 jab, for instance, was first developed as a strategy to tackle HIV because it triggers a strong immune response (SN: 2/27/21). The shot uses a common cold virus that has been altered so that it no longer causes disease. That carrier delivers instructions to cells to make the viral proteins needed to train the immune system to recognize the invader. Johnson & Johnson’s COVID-19 vaccine uses a virus called adenovirus 26; the first HIV vaccine candidates used adenovirus 5.
Unfortunately, a clinical trial to test the HIV vaccine showed that participants who had already been naturally infected with adenovirus 5 were more likely to become infected with HIV. Researchers halted the trial. They speculated that those participants were more susceptible to HIV because they already had immunity to adenovirus 5 and that dampened HIV-protective responses from the vaccine.

The absence of a good HIV vaccine is not for lack of trying, says Mark Feinberg, a viral immunologist who is president and CEO of the International AIDS Vaccine Initiative in New York City. “The work that’s gone into HIV vaccine development has been by far the most sophisticated and creative.”
Complexities of HIV
Much of the difficulty in making a vaccine comes from the complex biology of the virus itself.
One major challenge is the immense genetic diversity among HIV viruses infecting people around the world. Much like the coronavirus, which has variants that are more transmissible or able to evade parts of the immune system (SN: 1/27/21), HIV has variants too. But “it’s a completely different world for HIV,” says Morgane Rolland, a virologist with the Military HIV Research Program at the Walter Reed Army Institute of Research in Silver Spring, Md.
That’s because the virus makes new copies of its genetic blueprint at a dizzyingly fast rate, generating tens of thousands of new copies every day in a single person, Rolland says. Each of those new copies carries on average at least one unique mutation. Over the course of years, a single person can carry myriad variants in their body, though only a select few variants can be transmitted to others.
The main problem these variants pose for vaccines is that some mutations are in parts of the virus that the immune system tends to attack. Such changes can essentially help the virus go incognito. Good vaccines must spark an immune response capable of handling that vast diversity to provide broad protection against infection.
What’s more, the virus deploys multiple tactics to hide from the immune system. One tactic the virus uses is to cover parts of its surface in a dense layer of sugar molecules. Many of those surfaces would be the prime targets of immune proteins called antibodies that latch onto viral particles.
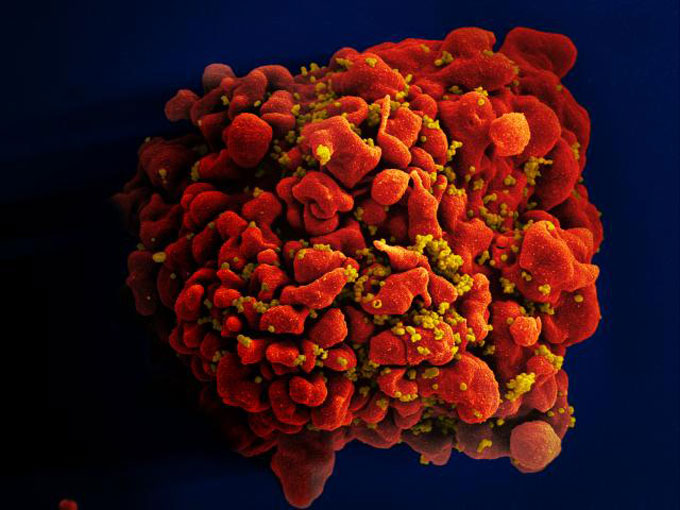
The body recognizes these sugars as “self,” says Barton Haynes, an immunologist at Duke University School of Medicine’s Human Vaccine Institute. “Basically, what the virus is saying to our immune system is ‘Sure, you can make a protective immune response, go for it.’” But if the antibodies attack, they’re seen as turncoats and are eliminated. That means the body can’t fight the virus as effectively.
Perhaps the biggest hurdle, however, is the lifelong nature of the infection. Many viruses disappear from the body after the immune system fights them off. But HIV has the ability to insert its genetic blueprint into host DNA, establishing a hidden reservoir in immune cells called T cells, which normally fight infections (SN: 10/24/13). That reservoir makes the virus invisible to the immune system. Once the virus inhabits its new hideout, the immune system can’t eradicate it, nor can drug treatments.
That means “you’ve got to have protective immunity there the day, the moment of transmission,” Haynes says. “If [the immune system] doesn’t get rid of the virus within 24 hours, the virus has won.”
Most vaccines don’t generate this type of sterilizing immunity that stops the infection from ever happening in most people who get the vaccine. Instead, shots are more likely to prevent people from becoming severely ill. Many COVID-19 vaccines, for instance, are highly effective at preventing people from developing symptoms, particularly severe ones. But some vaccinated people might still get infected with the coronavirus (SN: 5/4/21).
That’s not an option with HIV since it never leaves the body, Zolla-Pazner says. “It’s a very different bar that we have to jump over for an HIV vaccine.”
Testing HIV vaccine candidates
To date, there have been only a handful of clinical trials to test the efficacy of potential HIV vaccines in people. Of the six trials that scientists saw to completion, only one vaccine candidate proved effective at preventing infection.
That lone successful trial, known as RV144, used a “prime-boost” strategy in which participants received a total of six shots. The four “prime” jabs contained a canarypox virus that is incapable of replicating in cells and carries the genetic instructions for select HIV proteins. The participants’ cells make those viral proteins and develop an immune response against them.
Then participants also received two “boosts,” an injection of an HIV protein fragment that is essential for the virus to enter cells. The hope was that participants would develop a strong, wide-ranging immune response, giving those people broad protection against a variety of HIV subtypes.
Ultimately, that vaccine strategy lowered the risk of infection by 31.2 percent in vaccinated participants compared with the unvaccinated group. Although the shot showed only modest efficacy, those results changed the field by homing in on what type of immune response people needed to prevent infection, Zolla-Pazner says.
“Up until then, there was this raging debate about whether T cells or antibodies were most important in terms of protection,” Zolla-Pazner says. The results from RV144, first published in December 2009 in the New England Journal of Medicine, suggested specific antibodies were the crucial factor in reducing the risk of infection. “That’s not to say that T cells are not important — they are. But I think it established the primacy of antibodies,” she notes. If researchers could push people to make protective HIV antibodies, then perhaps a vaccine was within reach.
More recently, however, the canarypox/protein strategy has produced some less-promising results. In February 2020 — as COVID-19 was spreading around the globe — researchers stopped a follow-up trial being conducted in South Africa that used the same vaccine platform with the goal of improving on the RV144 finding (SN: 2/3/20). The results from the trial didn’t lower the risk of HIV infection in vaccinated people, researchers reported March 25 in the New England Journal of Medicine.
This is where more money for HIV vaccine research could have helped, Zolla-Pazner says. “If you had the money up front and you use it as needed… [scientists] would be doing science more efficiently and therefore getting the answers more quickly.” That investment is especially crucial for early animal testing. Instead of spending decades testing approaches on a handful of animals at a time to see if something works, an influx of money could support more robust experiments. And that could speed promising approaches into the arms of clinical trial volunteers.
Making the right immune response
There are now hopeful signs that vaccine developers working on a variety of platforms might be on the right track to make an effective shot that provides sterilizing immunity. Still, “I don’t think at this point we should be taking any approach off the table,” says Zolla-Pazner.
One approach is tapping into the idea that some infected people naturally make antibodies capable of attacking a wide assortment of HIV variants and stopping those viruses from infecting cells (SN: 7/20/17). These antibodies take a long time to develop. Sometimes they don’t develop until years after an HIV infection has taken hold, Haynes says. HIV vaccine-makers want to speed up the process.
There are several ways to do that. One, being tested now in a clinical trial led by Johnson & Johnson, is to spark a broad immune response using an HIV protein composed of a mosaic of different HIV strains circulating around the world. Another way is to teach the immune system to make broadly neutralizing antibodies.
To do that, researchers identify broadly neutralizing antibodies in people infected with HIV. Then they can analyze the steps the body took to create those immune proteins. The goal is to craft a vaccine that tells vaccinated people to make similar antibodies when exposed to specific viral fragments, says Kevin Saunders, a vaccinologist at the Duke Human Vaccine Institute.
In a December 2019 Science study, Saunders, Haynes and their colleagues showed that in vaccinated mice and rhesus macaques, they could spur the first steps of HIV antibodies that might eventually become broadly neutralizing. A separate effort by Feinberg and his colleagues recently showed that 97 percent of human participants in an early-stage clinical trial made those same rare immune cells when exposed to a piece of HIV engineered to specifically generate the cells.
Other groups are focusing on T cells to fight infection. Louis Picker and Klaus Früh, for instance, developed a vaccine that causes specialized T cells to kill other T cells infected with HIV, rather than relying on antibodies to prevent infection entirely, the team reported in March in Science Immunology.
The team had previously shown that around half of monkeys given the vaccine were protected. The animals became infected with SIV — the primate equivalent of HIV — but the virus couldn’t replicate very well and over time the infection went away, says Picker, an immunologist at Oregon Health & Science University in Portland.
The next step is to move the vaccine into people. “Whatever we see in the clinical trial, it’s breaking new ground,” says Früh, a viral immunologist also at Oregon Health & Science University. “It’s the first time this has ever been done so we’re very excited about that.”
After nearly four decades of trying, there is some light at the end of the tunnel. “I do believe we’ll get a vaccine, I really do,” Zolla-Pazner says. “But I don’t know how long that’s gonna take.”








